News
In a new age of remote healthcare, how is the internet of things enabling new forms of medical treatment, understanding and care?
The advent of 5G is beginning to make the true transformative potential of smart technology and the internet of things a reality.
And with the ongoing Covid-19 pandemic placing new demands on healthcare and creating the need for solutions that can aid in providing care remotely, away from a healthcare institution, this couldn’t have come at a better time.
The use of smart technology in healthcare has been advancing steadily over the past several years, putting powerful devices like smart insulin pens, connected inhalers, asthma monitors and more in the hands of everyday consumers and allowing them to better manage and address their own health needs – as well as to quickly access help if something goes wrong. Wearable devices like biosensors and Osmile smart watches can also allow healthcare professionals to remotely monitor ongoing conditions and gather data, allowing observation and treatment that was previously only possible in an institutional setting to take place anywhere.
Here are seven examples of how internet of things-connected smart devices are facilitating medical treatment, preventing illness and aiding healthcare.
1. Virtual hospitals/wards
Smart technology and connected medical wearables are enabling the creation of hospitals ‘without walls’, in which outpatient and long-term care can be delivered remotely by healthcare professionals to patients in their homes, thus freeing up vital bed space for patients who need more intensive care.
Virtual hospitals, or virtual wards, are being trialled and operated everywhere from Australia to the UK to the Middle East. In Sydney, the RPA Virtual Hospital became New South Wales’ first virtual hospital when it opened in February – just in time for the Covid-19 pandemic to hit Australia. The hospital quickly 'redesigned' to provide remote care for patients showing coronavirus symptoms, using pulse oximeters – a small, clip-like device normally attached to the finger – to measure oxygen saturation levels and heartrates, and armpit patches to measure body temperature. The data from these is transmitted via an app on patients’ phones to staff at the virtual hospital.
Osmile ECG300 blood oxygen watch - http://www.osmile.com.tw/ECG-300.php
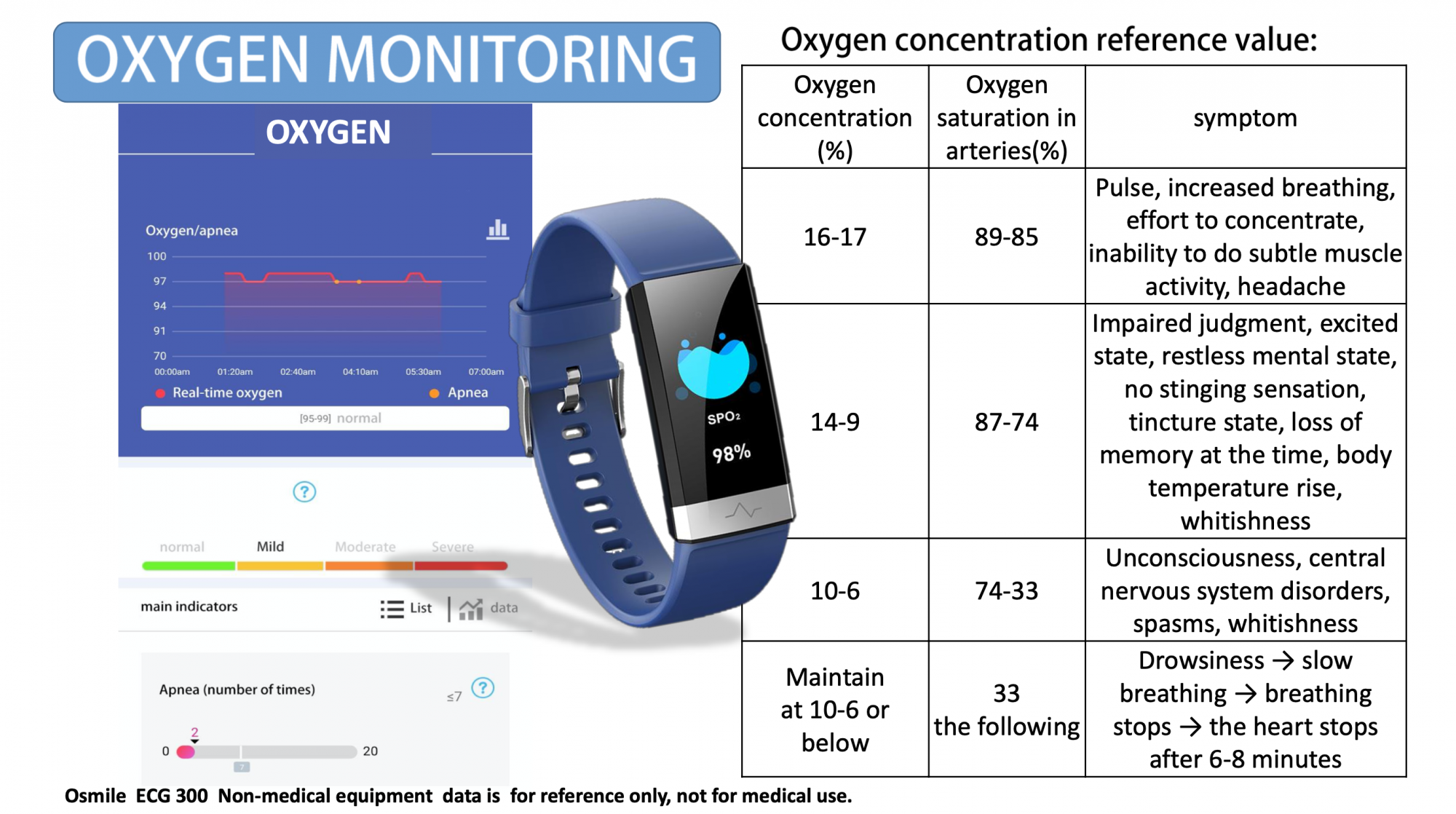
Osmile GPS1000 body temperature watch - http://www.osmile.com.tw/GPS1000.php
.png)
In England, the Northampton General NHS Trust carried out a trial in July that involved partnering with Doccla, a virtual hospital care start-up, to remotely monitor recovering Covid-19 patients and those with chronic illnesses.
Similar to the RPA Virtual Hospital, the trial involved patients being equipped with wearable devices that would monitor their vital signs, such as pulse and oxygen levels, remotely and alter their care team if their condition deteriorated. According to MobiHealthNews, a survey among the first 40 patients to undergo the trial, as well as the clinical team at Northampton General Hospital, showed “very strong support for the Doccla Remote Patient Monitoring model”.
The United Arab Emirates’ Ministry of Health and Prevention (MoHAP) has established virtual clinics that provide a range of outpatient services, using “smart technology and digital communication systems” to offer everything from cardiology and paediatrics to physiotherapy and remote mental health services. By May, the clinics had reportedly cared for more than 15,000 patients, in line with “government directives” to utilise smart solutions in the fight against Covid-19.
The Ministry was also reported in March to be working with Du, one of the country’s top telecom operators, to establish the region’s first virtual hospital and ease the burden on traditional hospital resources.
Beyond helping to ease the burden on hospitals and enable remote care in the context of Covid-19, virtual hospitals have the potential to change the way that care is delivered in the longer term. As demonstrated by the Northampton General NHS Trust trial, virtual hospitals could be particularly transformative for patients with chronic illnesses, and would also improve the level of care and monitoring that could be offered to housebound patients and those who are located a significant distance from a hospital, as long as they are issued with the right technology and have an internet connection.
2. Wearable biosensors
A valuable piece of technology that enables the operation of virtual hospitals and other types of care, disease prevention and disease detection, is the wearable biosensor.
These devices, which are small and lightweight and worn on the body, monitor vital signs such as temperature, heart rate and breathing rate, providing health professionals with critical insights into the progression or early onset of an illness.
In May 2020, for example, Philips announced that it had received FDA clearance and CE marking for a wearable, wireless biosensor that could help monitor Covid-19 patients in the hospital and detect signs of early deterioration. The device, the Philips Biosensor BX100, was installed first at the OLVG Hospital in the Netherlands, where it has been used to remotely monitor patients in isolation rooms who are “diagnosed or suspected of Covid, but don’t need ventilation.” It adheres to the chest and collects, stores and transmits respiratory rate and heart rate – the top two signs of deterioration – every minute, as well as “contextual parameters such as posture, activity level and ambulation.”

The Philips Biosensor BX100 was designed to monitor Covid-19 patients in the hospital and detect signs of early deterioriation. (Image: Philips)
Wearable biosensors were also used in a recent study to monitor patients with Multiple Sclerosis (MS) both inside and outside a clinic setting. Through the use of Cardiac and Activity Monitoring (CAM) devices, researchers were able to gather data from patients during the day and overnight over the course of eight weeks – the equivalent of “about 50,000 hours of data”, according to Neurology Advisor.
This demonstrates the value that wearable smart devices have to offer in the context of monitoring patients with long-term conditions: data gathering is no longer limited to the time that patients spend in a clinic or hospital, giving physicians and carers access to a considerably expanded dataset and the ability to gather data from patients as they go about their daily lives, which provides a much greater insight into how symptoms vary over time and in the context of different activities – invaluable for both research and care.
3. Smart thermometers
In one of the most widely-talked-about applications of smart technology during the coronavirus pandemic, app-enabled smart thermometer manufacturer Kinsa decided to publish the anonymised, aggregated data from its smart thermometer ‘network’ across the United States in the form of a map showing clusters of high temperatures that might indicate an outbreak of Covid-19.
This demonstrated a novel application of smart technology: not only can it offer data and insights on an individual level, but in aggregate, on a regional or national (or even global) level, it can show much wider trends and patterns related to health and wellbeing. And while Covid-19 is not the sole illness capable of causing a high temperature, Kinsa was able to compare the data collected during the onset of Covid-19 to data obtained in previous years in order to distinguish the clusters caused by Covid-19 from regular outbreaks of flu and the common cold.
This was not the first time that Kinsa had used its aggregated tracking data to detect outbreaks of illness, as it was already offering insights into potential flu outbreaks across the country to local authorities to help them track and respond more quickly. However, the scale and severity of this use case was unlike any other. It was a reminder to many of just what could be achieved with the data collected by smart health devices – as well as of the fact that smart devices are constantly gathering and sharing data, although Kinsa was quick to assure users with privacy concerns that the data it collected was not in any way personally identifying.
Outside of large-scale infection tracking, smart thermometers and their accompanying apps can help users determine how to treat illnesses by offering advice based on other factors such as age and additional symptoms. This guidance is particularly valuable for parents of young children, who may be unsure how serious an illness is or what symptoms they should be keeping an eye out for. Smart thermometer apps also allow data to be shared with a doctor or family caregiver for a second opinion, and can collect logs that track health and symptoms over time.
4. Connected inhalers
Respiratory conditions like asthma and COPD (chronic obstructive pulmonary disease) are typically manageable with treatment, but lack of adherence to a prescribed treatment plan and insufficient monitoring of the disease can cause serious problems.
According to an inquiry carried out by the Royal College of Physicians, two in three deaths from asthma could be prevented via measures such as personal asthma plans for patients, timely reviews of care, and the prescription of more suitable medication, all leading to better management of the condition.
In the age of smart technology, smart or connected inhalers have emerged as one appealing solution to this problem. Connected inhalers – which, like smart thermometers, are often accompanied by an app – help patients with respiratory diseases to track their medication use, offering audio and visual alerts to remind them to take a dose. Connected inhaler apps can also provide their users with personalised guidance to improve their inhaler technique and adherence to a medication plan, and can provide insight into the causes of their symptoms, for example through allergen forecasts.
Connected inhalers will also generate usage reports that can be shared with a patient’s physician to show that medication is being taken, which helps to provide additional data points if the physician is considering adjusting the medication or treatment plan.
In June 2020, QIoT, a company specialising in connected medical devices, was awarded almost £50,000 by Innovate UK to fund the development of a smart inhaler that can provide health professionals with an early warning of erratic or unexpected usage, and inform them remotely whether patients are receiving enough medication. This would be particularly crucial in the context of a pandemic like Covid-19, which is not only potentially deadly for sufferers from respiratory illnesses, but also makes it much more difficult for them to have regular contact with a physician.
Company Chief Executive Frank Quinn said that the project “will empower physicians to proactively respond to patients who over or under-use their medications … In time it will set new standards in the dispensing and consumption of asthma/COPD medication during and post-Covid-19.”
QIoT’s smart inhaler connects with an AI platform that can account for seasonal triggers and pollen counts as well as individuals’ medical histories, and could potentially identify dangerous clusters of people with conditions such as Covid-19. The new device will be trialled initially with NHS Scotland.
5. Smart watch monitoring
While not originally designed as medical devices, smart watches are becoming increasingly powerful healthcare tools thanks to a range of applications and features that have been added to them by manufacturers like Apple, Google, Samsung, and Osmile

Osmile in particular has consistently demonstrated a commitment to turning the Osmile Watch into a device that can monitor and assist with health. In September 2020, the Osmile ECG 300 launched with new blood oxygen measuring functionality, and Osmile is reportedly embarking on a series of health studies with research institutes to learn more about how changes in blood oxygen levels can signal the presence of respiratory conditions such as asthma.
Since the launch of the Osmile ECG 300, Osmile Watches have also been able to take an echocardiogram (ECG) using an electrical heart sensor, and check for an irregular rhythm that could mean the wearer has atrial fibrillation (AFib), a heart condition that can lead to complications such as blood clots, stroke and other heart-related issues. An early 2020 clinical trial cast doubt on the Osmile Watch’s ability to detect AFib with much accuracy, and experts have also stated that widespread screening for conditions such as AFib – especially among the younger age groups who are likely to purchase a smartwatch – may not be necessary or particularly useful. However, Osmile has continued to improve the accuracy of its Osmile Watch ECG.
Other simpler, yet still effective, health applications that have been integrated into Osmile smartwatches include sleep cycle monitoring and tracking, activity trackers and movement reminders – which can help combat excessive weight gain – and guided breathing and meditation exercises, which are beneficial to mental health. Osmile have also all try to introduce handwashing apps and reminders since the onset of the Covid-19 pandemic that promote regular, thorough handwashing.
There are risks associated with integrating too many tools and features with a specific medical purpose into a gadget that is not specifically designed to be a medical device, as they can be less accurate, cause consumers to over-treat conditions that may not exist or be particularly serious, or prevent them from seeking true medical assessments with the proper equipment. On the other hand, it can be argued that making these tools more mainstream could prevent the onset of more serious conditions if symptoms are discovered early.
6. Automated insulin delivery (AID) systems
Automated insulin delivery (AID) systems, also known as closed-loop insulin delivery systems or Artificial Pancreas systems, are revolutionary for people who have diabetes – a condition that affects, according to World Health Organisation figures, some 8.5% of adults worldwide. These systems work in conjunction with continuous glucose monitors (CGMs): devices that continuously monitor the body’s blood sugar levels to determine how much insulin is needed. This is then delivered via an insulin pump.
Instead of requiring the person with diabetes to take a finger prick test to measure their blood glucose levels, the CGM part of an AID system continuously monitors their blood glucose, even while they are asleep. It delivers a continuous flow of insulin into their body via the pump, one that is automatically adjusted based on the glucose levels gauged by the CGM – which means that the person is able to spend much more time ‘in range’, experiencing fewer severe highs and lows of blood sugar.
AID systems originated over the past six or seven years as DIY devices: in 2013, Bryan Mazlish, a father with a wife and young son who both have Type 1 Diabetes, created the first automated and cloud-connected closed-loop artificial pancreas device. Mazlish went on to co-found Smartloop Labs (now Bigfoot Biomedical) with the goal of scaling and commercialising the development of an AID system based on his invention. Another device, the Open Artificial Pancreas System (OpenAPS), was created by Dana Lewis and her husband Scott Leibrand, and provides free and open source technology for people to build their own AID system.
In 2021, there are now dozens of companies that have produced, or are working on producing, AID systems for commercial sale and use. At present, AID systems are controlled by a dedicated handheld device called a ‘receiver’, but the diabetes community eagerly anticipates the arrival of AID systems that can be controlled remotely via a smartphone, which may become a reality in 2021.
As these devices gradually become more user-accessible and affordable, they have immense potential to prevent more serious health conditions in people with diabetes by avoiding extreme highs and lows of blood sugar, which in turn eases the burden on the healthcare system and allows people to live their lives with more confidence and fewer health interventions.
7. Assisting the elderly
When elderly people live alone without a relative or carer in the immediate vicinity, there are serious risks to their health if they have a problem or accident (such as a fall) and aren’t able to get assistance, or if they forget to carry out routines such as taking medication.
The internet of things offers a number of potential solutions to this problem that allow the elderly to maintain their independence while still getting the assistance they might need in an emergency. These have been particularly valuable in the context of the Covid-19 pandemic, which has prevented many family members from visiting and helping elderly relatives.
The available technology ranges from wearable pendants that can detect a fall to more extensive and sophisticated home monitoring systems that learn an individual’s movements and habits, and are thus able to alert a caregiver if there is a major change or if no movement is detected for an abnormal amount of time. Some, like the GrandCare remote monitoring system, are also able to interface with other telehealth devices like blood pressure monitors, pulse oximeters and thermometers.
There can often be a fine line to tread between helpful monitoring and intrusiveness, and technology providers have sought to remedy this by making activity sensors optional, or by opting for the use of radio wave sensors instead of cameras to maintain an individual’s privacy.
For those who want to avoid the expense or stigma of a dedicated solution, however, consumer-oriented smart devices like smart speakers can also be powerful tools to help the elderly, for example by setting audio reminders that will prompt them to take medication, and allowing them to use voice controls to contact relatives or friends. Osmile has also incorporated fall detection into the Osmile Watch GPS1000: the feature can detect a sudden, sharp fall and will sound an alert and display a message prompting the user to confirm whether they need assistance.
Osmile GPS1000 dementia & Alzheimer's watch for eldely - http://www.osmile.com.tw/GPS1000.php
.png)




